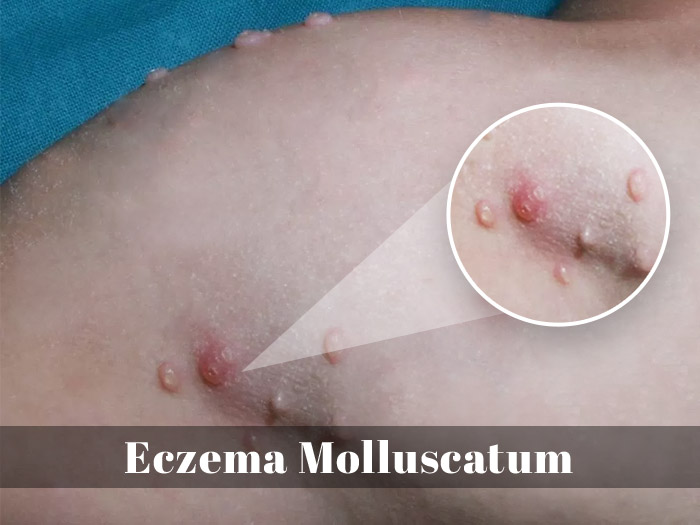
Eczema molluscatum describes the occurrence of molluscum virus infection in a patient with underlying atopic dermatitis. Novel, safe and effective treatment options in atopic dermatitis are the topical immunomodulators tacrolimus and pimecrolimus. One major advantage over corticosteroids is that they do not induce skin atrophy. Some physicians fear that topical immunomodulators may predispose patients to skin infections.
What is eczema?
Eczema Or (Atopic Dermatitis) is a chronic condition that causes the affected skin patch to become itchy, red, dry, scaly and even cracked in severe conditions. This common skin condition is usually diagnosed in children, however, the adults may also develop it.
Although, no specific cause has so far been diagnosed behind the occurrence of this ailment, family history of asthma, hay fever, eczema and other allergies, genes are often linked with eczema.
There are certain triggers that are considered to worsen the symptoms of eczema. The triggers vary for different individuals, but in most cases, stress, environmental factors, certain classes of foods, pollens, detergents, fabrics can result in flare-ups.
Know more about various types of eczema:
Contact Dermatitis | Weeping Eczema | Eczema on Lips | Eczema In Babies | Dyshidrotic Eczema | Eczema on Hands | Follicular Eczema | Eczema on Ear | Eczema on Eyes | Nummular Eczema | Eczema on Face | Perioral Dermatitis
What is Eczema Molluscatum?
Eczema weakens the skin barrier mechanism, making it more susceptible to viral infection. In addition to Eczema herpeticum, people with Atopic Dermatitis are more likely to get infected by the virus, Molluscum contagiosum that causes a skin condition which is often confused with eczema due to its appearance.
When eczema and Molluscum contagiosum occur together, it is referred to as eczema molluscatum (EM). Before understanding the term in detail, let’s consider the basics with respect to molluscum contagiosum.
What Is Molluscum Contagiosum?
Molluscum contagiosum is a skin infection named after the virus that causes it. The viral infection results in the formation of benign raised lesions or bumps on the outer layer of the dermis.
These bumps are normally painless and mostly disappear on their own while, leaving no scars. The timespan for which the virus remains in the body varies for individuals, however, the bumps may appear for a duration of two months to as long as four years.
While, eczema is a non-contagious skin condition, Molluscum contagiosum is communicable infection that spreads by coming in contact with the infected person or by using their contaminated objects, such as a towel or a piece of clothing.
The virus easily affects those with a weakened immune system. Rather, it becomes difficult to treat the condition, if the body’s immune system doesn’t function effectively.
Pictures of Molluscum Contagiosum
What Are the Symptoms of Eczema Molluscatum?
It may take up to six months for the Molluscum Contagiosum symptoms to appear after you or your child has been infected by the virus, M. contagiosum. The average incubation period is between two and seven weeks.
The initial signs may include the appearance of a small group of painless bumps. Depending upon the severity of the condition, these lesions may appear alone or in a group. The blisters or lesions are usually:

- very small, shiny, and smooth in appearance
- flesh-colored, white, or pink
- firm and shaped like a dome
- large with the indented centers
- filled with a central core of waxy material
- between 2 to 5 millimeters in diameter
- appear anywhere except on the palms of your hands or the soles of your feet
- affect the face, abdomen, torso, arms, and legs
- appear on the inner thigh, genitals, or abdomen in adults
However, the ones with a very weak immune system are likely to develop more significant symptoms. The lesions may appear larger in size. The bumps may specifically affect the face and be resistant to treatment.
Who are at risk of getting Eczema Molluscatum?
Although, the viral infection can affect people of any age and sex, certain groups of people are at more risk of getting infected. These groups include:
- children aged between 1 and 10
- people with atopic dermatitis
- people who live in warm, humid climates with crowded living conditions
- people with a weak immune system resulting because of HIV, organ transplants, cancer treatments or similar ailments
- teens and young adults usually get infected by sexual contact
- people who participate in sports that includes bare skin-to-skin contact, such as wrestling or football, swimming, gymnastics
- massage therapists, people who use steam rooms and saunas can also carry this infection
How are Molluscum and Eczema related to each other?
Although, the relationship between the molluscum contagiosum virus (MCV) and atopic dermatitis (AD) is unclear, they share a few common elements that tend to affect the overall skin condition of an individual.
More specifically children with eczema are susceptible to be infected with this virus. On an average, 10% of individuals with papules or lesions develop eczema around them.
Atopic Dermatitis results in extensive itching forcing you to scratch the papules. The scratched skin makes it easy for the virus to penetrate and infect the already affected area.
When an individual affected with eczema develops a severe skin condition after being infected by the virus, it is known as eczema molluscatum (EM).
Following the infection, itching and scratching of the lesions results in further spreading to other broken skin patches. In a few cases, it has been found that cortisone creams (used to treat eczema) subdue the immunity of the skin, resulting in the formation of more lesions.
Hence, your dermatologist may recommend to treat the bumps before eczema to manage the skin conditions. A few cases of EM have reported success after being treated with 0.1% tacrolimus ointment, a steroid that reduces inflammation.
Eczema Molluscatum Treatment (EM)?
 Sources : https://www.gstatic.com/healthricherkp/pdf/molluscum_contagiosum_en_IN.pdf
Sources : https://www.gstatic.com/healthricherkp/pdf/molluscum_contagiosum_en_IN.pdf
Adoption of necessary precautionary measures is the foremost aspect to undertake while treating this condition. A few of the measures include:
- It is essential that people with this condition don’t share baths and personal toiletries such as soap, hair brushes, clothes, towels, or razors.
- Their workout equipment should be properly cleaned before and after they use it.
- They must wash their hands regularly and properly, and practice safer sex
- They should avoid scratching irritated skin to make to prevent the MCV from penetrating the skin and replicating itself.
Molluscum contagiosum can only be treated once it has been diagnosed based on the appearance of the papules and/or examination of the material extracted from the centre of a lesion.
The diagnosis can’t be performed before an outbreak occurs. Additionally, the incubation period for the virus can be months long, hence, it is advisable to follow the precautionary measures in order to avoid the severe conditions.
Although, molluscum contagiosum is more common in case of people with eczema, few other skin problems like warts (genital or otherwise), herpes, pearly penile papules, are often confused with the papules.
It is highly recommended that you seek medical advice for proper diagnosis of the skin.
Author Bio:
Shaliza Gill is a Content Writer, Manager, and Developer, producing content, including infographics, websites, and blogs. She has completed her Master of Science in 2013 and has been managing content at Eczema Living since 2015. She coordinates teams of writers, editors, and project managers. Her goal is to produce content that is thoroughly researched, clearly explained, and as helpful as possible to the readers.